Disrupting malaria’s inner balance: targeting parasite’s protein control system could be key to innovative treatments
IBEC and ISGlobal researchers led a study that points towards protein aggregation as a possible target to find new ways to reduce the viability of Plasmodium falciparum, the main causing agent of malaria. By inducing protein aggregation, they observed considerable disorders in protein homeostasis and a significant reduction in parasite growth. The results position protein aggregation control as a promising target for antimalarial therapies.




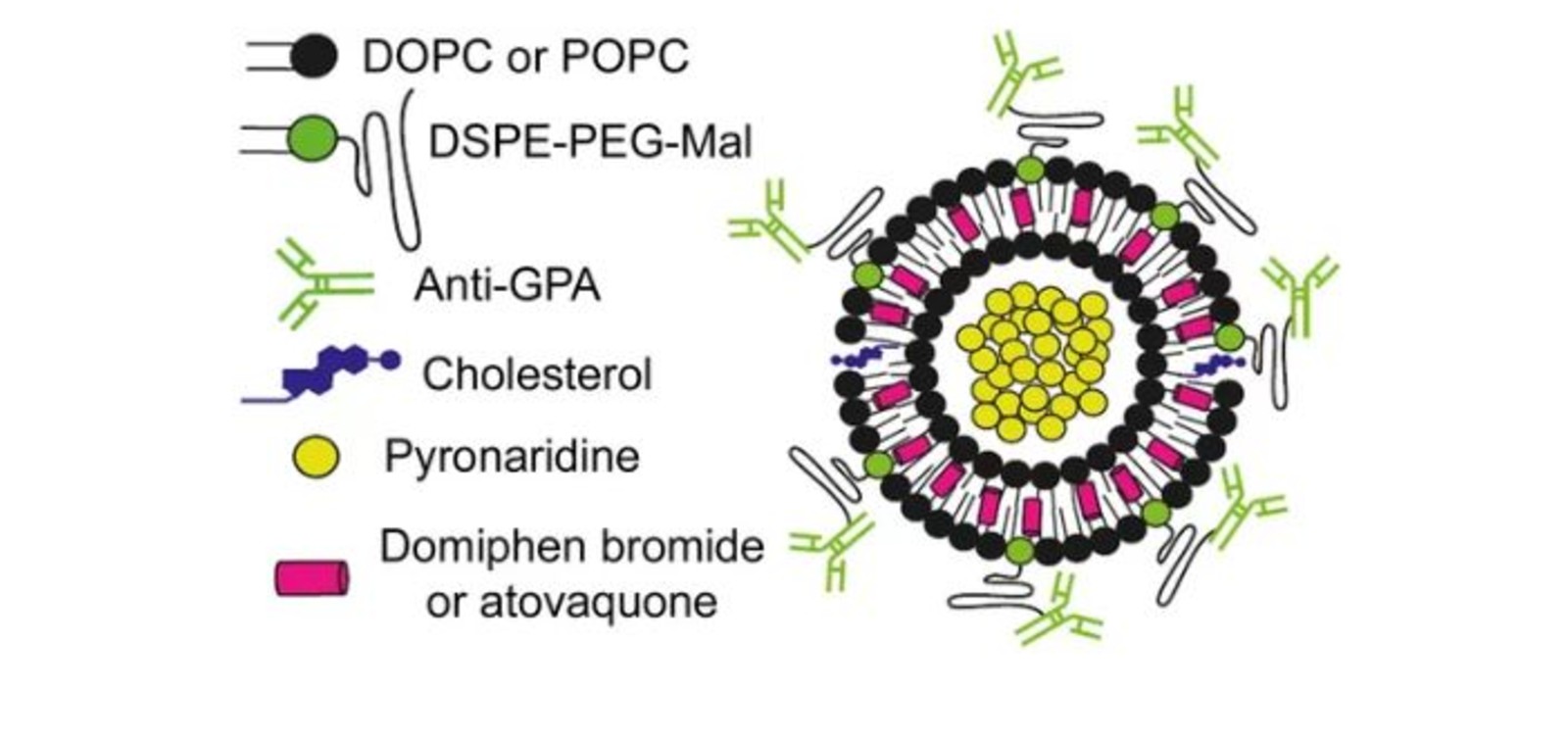
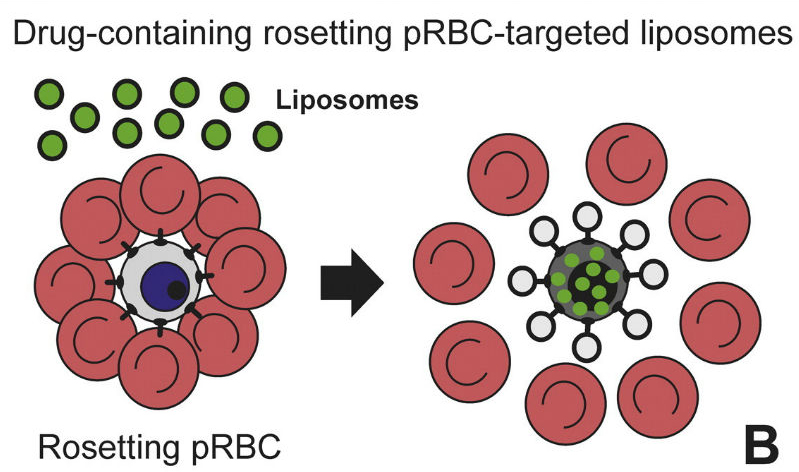
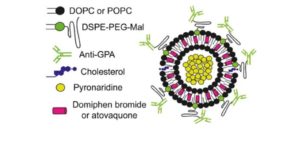 According to the study, the strategy has the added advantage of targeting the transmissible phase of the parasite- the gametocyte. Encapsulating two drugs with different properties into nanovesicles surrounded by antibodies can greatly improve their delivery and efficacy, according to a study led by Xavier Fernández Busquets, director of the joint Nanomalaria unit at the Institute for Bionengineering of Catalonia (IBEC) and the Barcelona Institute for Global Health (ISGlobal), an institution supported by ”la Caixa”.
According to the study, the strategy has the added advantage of targeting the transmissible phase of the parasite- the gametocyte. Encapsulating two drugs with different properties into nanovesicles surrounded by antibodies can greatly improve their delivery and efficacy, according to a study led by Xavier Fernández Busquets, director of the joint Nanomalaria unit at the Institute for Bionengineering of Catalonia (IBEC) and the Barcelona Institute for Global Health (ISGlobal), an institution supported by ”la Caixa”. 
 Projects led by IBEC group leader Xavier Fernandez-Busquets and Associated Researcher Antonio Juarez have received funds from 2017’s La Marató de TV3 fundraising campaign.
Projects led by IBEC group leader Xavier Fernandez-Busquets and Associated Researcher Antonio Juarez have received funds from 2017’s La Marató de TV3 fundraising campaign.